Ever wonder why that third drink sounds like a fantastic idea when you're stressed? Turns out, your brain has been running a secret communication network between its anxiety headquarters and the control room for habits and decisions. And alcohol? It's been eavesdropping on the line.
The Brain's Unlikely Power Couple
Meet the extended amygdala - specifically the central amygdala (CeA) and bed nucleus of the stria terminalis (BNST). Think of these regions as your brain's drama department, constantly broadcasting stress signals via a molecule called corticotropin-releasing factor, or CRF. This stuff is basically the neurochemical equivalent of your coworker who CC's everyone on panic emails.
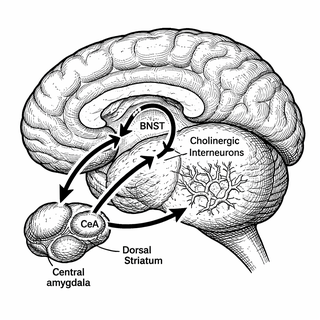
Now meet cholinergic interneurons (CINs) in the dorsal striatum. Despite making up only 1-2% of striatal neurons, these cells are the ultimate overachievers. They release acetylcholine, which helps your brain switch gears, update behaviors, and generally not get stuck doing the same dumb thing over and over. They're like the IT department of your decision-making process.
A team led by Jun Wang at Texas A&M and collaborators decided to investigate whether these two systems were talking to each other - and boy, were they.
Wait, There's a Direct Line?
Using some impressively sophisticated circuit tracing (imagine GPS tracking for neurons), the researchers discovered that CRF-expressing neurons from both the CeA and BNST send direct projections to those hardworking cholinergic interneurons in the dorsal striatum. The BNST, it turns out, is particularly chatty - providing substantially more connections than the CeA.
Here's where it gets interesting: when CRF activates these interneurons, it cranks up their excitability and promotes acetylcholine release. Translation? Stress signals from your anxiety centers are supposed to help your decision-making circuits stay sharp and flexible. It's like your brain's way of saying "Hey, things are getting real - pay attention and adapt."
But alcohol throws a wrench into this whole operation.
Alcohol: The Ultimate Conversation Killer
When the researchers exposed the circuit to alcohol - both during acute intoxication and withdrawal - something concerning happened. The CRF-induced boost to cholinergic interneurons got significantly dampened. The stress signal was still being sent, but the message wasn't getting through properly.
Think of it like this: your brain's stress alarm is ringing, but alcohol put a pillow over the speaker. The interneurons that should be helping you adapt and change course? They're not getting the memo.
This matters because cholinergic interneurons are essential for behavioral flexibility - your ability to stop doing something that's no longer working and try something new. When this system gets compromised, you're more likely to get stuck in rigid, habitual patterns. Like, say, reaching for another drink even when you know you shouldn't.
Why This Research Actually Matters
Alcohol use disorder affects roughly 29.5 million Americans, and relapse rates remain stubbornly high. We've known for years that CRF and stress play major roles in driving people back to drinking, but the precise mechanisms have been murky.
This study illuminates a specific circuit - a actual anatomical pathway - that connects stress processing to the brain regions governing habits and decision-making. By showing that alcohol specifically disrupts CRF signaling to cholinergic interneurons, the researchers have identified a potential target for future treatments.
Previous work has established that CRF antagonists can reduce excessive drinking in alcohol-dependent animals, and that the extended amygdala is critical for addiction-related behaviors. This new research adds an important piece to the puzzle by showing exactly how stress signals reach the striatal circuits that control our habits.
The Bottom Line
Your brain evolved an elegant system: stress activates the extended amygdala, which sends CRF signals to boost the cholinergic interneurons that help you adapt your behavior. It's supposed to help you navigate challenging situations with flexibility and smarts.
Alcohol, however, gums up this whole process. By attenuating the CRF-to-CIN signal, it may promote the kind of rigid, compulsive behavior that characterizes addiction. The stressed brain tries to call for backup, but the message keeps going to voicemail.
Understanding this circuit doesn't just satisfy scientific curiosity - it opens doors to interventions that might help restore normal communication and give people struggling with alcohol use disorder a better shot at recovery.
References:
-
Essoh A, Xie X, Gangal H, et al. (2025). Alcohol attenuates CRF-induced excitatory effects from the extended amygdala to dorsostriatal cholinergic interneurons. eLife. DOI: 10.7554/eLife.107145
-
Heilig M, Koob GF. (2007). A key role for corticotropin-releasing factor in alcohol dependence. Trends in Neurosciences. PMCID: PMC2747092
-
Jennings JH, et al. (2013). Distinct extended amygdala circuits for divergent motivational states. Nature. PMCID: PMC3858407
-
Gonzales KK, Smith Y. (2015). Cholinergic interneurons in the dorsal and ventral striatum: anatomical and functional considerations in normal and diseased conditions. Annals of the New York Academy of Sciences. PMCID: PMC4564338
-
Zorrilla EP, et al. (2014). Corticotropin Releasing Factor: A Key Role in the Neurobiology of Addiction. Frontiers in Neuroendocrinology. PMCID: PMC4213066
Disclaimer: The image accompanying this article is for illustrative purposes only and does not depict actual experimental results, data, or biological mechanisms.
