I'll be honest - writing about obesity research is a minefield. Half the internet is selling you miracle cures, and the other half is dunking on miracle cures. So when a study comes along that genuinely changes what we know about how a hormone burns fat in the brain, the challenge is getting you to stick around long enough to hear it out.
Here's why you should: this one's actually wild.
Your Brain Has a Backroom You Didn't Know Was Running Things
So there's this hormone called FGF21 (fibroblast growth factor 21, if you're keeping score). Scientists have known for years that pumping it into obese mice makes them lose weight - not by killing their appetite, but by cranking up their metabolic rate. Think of it as turning up the thermostat instead of locking the fridge. The problem? Nobody could figure out where in the brain FGF21 was pulling the levers.
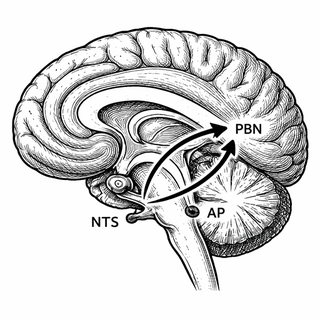
Most researchers assumed the hypothalamus was the star of the show. It's basically the brain's metabolic control room - temperature, hunger, energy balance, all the greatest hits. But a team led by Matthew Potthoff at the University of Oklahoma just flipped the script in a new Cell Reports study (Lin et al., 2026). The real action? It's happening in the hindbrain - specifically in two tiny regions called the nucleus of the solitary tract (NTS) and the area postrema (AP).
The Hindbrain: Your Brain's Underrated Middle Manager
Look. The hindbrain doesn't get a lot of press. It's back there handling basics like breathing and blood pressure while the cortex hogs all the "consciousness" headlines. But the NTS and AP sit in a unique spot - they're part of the few brain areas where the blood-brain barrier is leaky on purpose, meaning they can directly sample what's floating around in your bloodstream. Hormones, toxins, that questionable gas station sushi - these regions are your brain's first responders.
The researchers found that neurons in the NTS and AP express beta-klotho (KLB), which is FGF21's VIP pass into cells. Without KLB, FGF21 is basically knocking on a door nobody answers. When the team knocked out KLB specifically in these hindbrain neurons, FGF21 lost its weight-loss superpowers entirely. When they activated only these neurons? The mice burned more energy and dropped weight even without FGF21. These cells aren't just involved - they're running the whole operation.
Plot Twist: It's Not About the Hypothalamus
Here's where it gets really interesting. The NTS/AP neurons don't just sit there soaking up FGF21 signals - they make a phone call. And the number they're dialing isn't the hypothalamus (the brain region everyone expected). Instead, they're ringing up the parabrachial nucleus (PBN), a relay station deeper in the brainstem that's been getting more attention lately for its role in feeding behavior and energy regulation (Owen et al., 2014).
The researchers used some elegant circuit-tracing techniques to show that KLB neurons projecting from the NTS/AP to the PBN are both necessary and sufficient for FGF21's metabolic effects. Cut that wire, and the whole system goes dark. The hypothalamus connection? Turns out it's more like a CC on an email nobody reads.
Why This Isn't Just Another Mouse Study
Here's the thing. You've probably heard about GLP-1 drugs like Ozempic and Mounjaro - they've basically taken over the obesity conversation. Those drugs work by crushing your appetite, targeting some of the same hindbrain regions. But FGF21 plays a completely different game. Instead of making you eat less, it makes your body burn more. It cranks up sympathetic nerve activity to brown fat, essentially telling your body to convert calories into heat (Owen et al., 2014).
That distinction matters enormously. GLP-1 drugs come with side effects like nausea, muscle loss, and the fun reality that you regain weight when you stop taking them. FGF21 analogues are already in clinical trials for MASH (metabolic dysfunction-associated steatohepatitis, a severe form of fatty liver disease), and early results show they improve liver fat, fibrosis, and metabolic markers. Some researchers are even exploring GLP-1/FGF21 combo therapies - one suppresses appetite while the other revs metabolism - for potentially more durable weight loss (Gilroy et al., 2020).
The Big Picture
This study maps a precise neural circuit - from hindbrain to parabrachial nucleus - that FGF21 uses to burn energy and reverse obesity. That's not just academically cool; it's a roadmap for drug design. If you know exactly which neurons to target, you can build smarter, more precise therapies with fewer side effects. Beta-klotho's role as the gatekeeper makes it a particularly attractive drug target (Aaldijk et al., 2023).
We're still in the early chapters of this story. But for the first time, we have a clear picture of FGF21's neural wiring diagram - and it was hiding in the brain's back office the whole time.
References
-
Lin, Y., Claflin, K.E., Aklan, I., Morgan, D.A., Sullivan, A.I., Rudolph, M.C., Rahmouni, K., & Potthoff, M.J. (2026). Pharmacological administration of FGF21 reverses obesity through a parabrachial-projecting neuron population in the hindbrain. Cell Reports, 44(4), 117093. DOI: 10.1016/j.celrep.2026.117093 | PubMed
-
Owen, B.M., Ding, X., Morgan, D.A., Coate, K.C., Bookout, A.L., Rahmouni, K., Kliewer, S.A., & Mangelsdorf, D.J. (2014). FGF21 acts centrally to induce sympathetic nerve activity, energy expenditure, and weight loss. Cell Metabolism, 20(4), 670-677. DOI: 10.1016/j.cmet.2014.07.012 | PMCID: PMC4192037
-
Aaldijk, A.S., Verzijl, C.R.C., Jonker, J.W., & Struik, D. (2023). Biological and pharmacological functions of the FGF19- and FGF21-coreceptor beta klotho. Frontiers in Endocrinology, 14, 1150222. DOI: 10.3389/fendo.2023.1150222 | PMCID: PMC10229096
-
Gilroy, C.A., Capozzi, M.E., Varanko, A.K., Tong, J., D'Alessio, D.A., Campbell, J.E., & Chilkoti, A. (2020). Sustained release of a GLP-1 and FGF21 dual agonist from an injectable depot protects mice from obesity and hyperglycemia. Science Advances, 6(35), eaaz9890. DOI: 10.1126/sciadv.aaz9890 | PMCID: PMC7449677
Disclaimer: The image accompanying this article is for illustrative purposes only and does not depict actual experimental results, data, or biological mechanisms.
