Imagine waking up every day with a mind that works against you. Not in the obvious ways - you can walk, talk, and hold a conversation. But something's off. You struggle to remember whether you turned left or right to get to the grocery store last week. Holding multiple pieces of spatial information in your head feels like juggling water. For people living with 22q11.2 deletion syndrome, this cognitive fog isn't occasional; it's constant. About 1 in 4,000 people carry this genetic condition, and roughly one in four of them will develop schizophrenia. Understanding why their brains struggle with spatial memory isn't just academic curiosity - it's the first step toward helping them.
The Brain's Secret Long-Distance Calls
Your hippocampus - that seahorse-shaped structure nestled deep in your temporal lobe - runs your brain's GPS and memory filing system. Within it sits a region called CA1, which acts as the hippocampus's primary output station. Scientists have known for decades that the two sides of your brain communicate through a bundle of nerve fibers called the commissure. But here's what's surprising: we thought we had the hippocampus's communication network pretty well mapped out. Turns out, we missed a line.
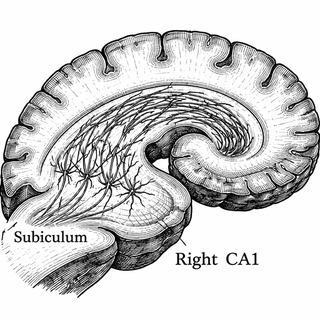
Researchers led by Félix Leroy at the Instituto de Neurociencias in Spain, working with colleagues at Columbia University, discovered that neurons in the right dorsal CA1 region don't just chat with their immediate neighbors. They send long-distance projections all the way across to the subiculum on the left side of the brain. The subiculum serves as the hippocampus's major exit ramp, channeling processed information to the rest of the brain. Think of it as discovering that your office's quiet corner cubicle has been secretly running a transatlantic phone line this whole time.
What Happens When the Connection Breaks
The research team didn't just find these connections - they tested what they actually do. Using optogenetics (essentially giving scientists a remote control for specific neurons), they selectively silenced this right-to-left pathway in mice. The result? The animals stumbled on tasks requiring them to remember locations and hold spatial information in working memory.
Here's where things get clinically relevant. The Df16(A)+/- mouse model mimics 22q11.2 deletion syndrome - the same genetic condition that dramatically raises schizophrenia risk in humans. When the team examined these mice, they found something striking: the interhemispheric projections from right CA1 to left subiculum were significantly reduced. Male mice showed particularly severe anatomical deficits.
This finding adds a piece to a puzzle that's been vexing psychiatrists for years. Spatial working memory problems show up reliably in people with schizophrenia and in those at genetic risk for the disorder. A 2008 study identified spatial working memory as a potential endophenotype - a biological marker that bridges genes and illness. But we didn't know which specific circuits were involved. Now we have a candidate.
Why Right to Left?
The brain isn't symmetrical in function, even if it looks roughly mirror-imaged. The right hippocampus appears to play a special role in integrating information from both hemispheres before sending it to the cortex. Research published in Nature Communications showed that the interhemispheric CA1 circuit governs how mice generalize learned fears to new situations. Disrupting these connections uncouples the synchronized brain waves that seem to underlie coherent thought.
The subiculum, meanwhile, isn't just a passive relay station. Studies show it encodes navigational information - position, speed, movement direction - often with higher accuracy than CA1 itself. It also lights up during sleep replay, when the brain consolidates spatial memories. A broken line from CA1 to the subiculum isn't just one faulty wire; it's a disruption of the brain's spatial memory consolidation system.
The Bigger Picture
Current antipsychotic medications do almost nothing for the cognitive symptoms of schizophrenia. Clinical research consistently shows that while these drugs can quiet hallucinations and delusions, they leave working memory deficits largely untouched. And cognitive impairment, not psychotic symptoms, is what best predicts how people with schizophrenia will function in daily life.
Having a specific circuit to target changes the game. If we understand exactly which connections fail in 22q11.2 deletion syndrome, we can begin asking whether strengthening or protecting those connections might help. This research won't lead to a treatment tomorrow, but it points toward a more precise future - one where we might intervene before the cognitive decline becomes entrenched.
For now, the finding is a reminder of how much the brain still has to teach us. A pathway we didn't know existed turns out to matter enormously. Somewhere between your brain's two hemispheres, a conversation is happening that keeps you oriented in the world. When that conversation breaks down, so does something fundamental about how we navigate our lives.
References:
-
de León Reyes NS, et al. (2026). Interhemispheric CA1 projections to the subiculum support spatial cognition and are affected in a mouse model of the 22q11.2 deletion syndrome. Cell Reports, 45(4):117114. DOI: 10.1016/j.celrep.2026.117114
-
Finlay JM, et al. (2015). The subiculum: Unique hippocampal hub and more. Neuroscience & Biobehavioral Reviews. PMID: 30121285
-
Zhou H, et al. (2017). The interhemispheric CA1 circuit governs rapid generalisation but not fear memory. Nature Communications. DOI: 10.1038/s41467-017-02315-4
-
Barch DM, Ceaser A. (2012). Treating Working Memory Deficits in Schizophrenia: A Review of the Neurobiology. Biological Psychiatry. Link
-
Glahn DC, et al. (2003). Spatial working memory as a cognitive endophenotype of schizophrenia: assessing risk for pathophysiological dysfunction. Schizophrenia Bulletin. PMID: 16687386
Disclaimer: The image accompanying this article is for illustrative purposes only and does not depict actual experimental results, data, or biological mechanisms.
